More and more people are seeing that cholesterol alone does not tell you enough about whether you are actually at increased risk for cardiovascular disease.
People are often quick to reach for statins, but it is advisable to take a deeper look at cholesterol, which may have caused any elevation.
Is ApoB a better predictor of cardiovascular disease risk?
Although cholesterol has long been considered an important risk factor for cardiovascular disease, it is increasingly recognized that measuring apolipoprotein B (ApoB) may be a better indicator of risk for these conditions.
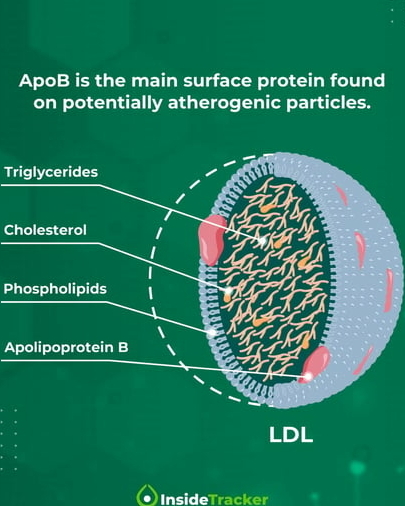
ApoB is a protein found on the LDL cholesterol particles (also called "bad" cholesterol) circulating in the blood. LDL cholesterol is able to bind to the blood vessel wall and accumulate in it. This accumulation can lead to thickening and hardening of blood vessels, restricting blood flow to the heart and other organs and increasing the risk of cardiovascular disease. ApoB is therefore a better indicator of the total number of LDL particles in the blood than measuring LDL cholesterol alone.
There are several reasons why measuring apoB may be a better predictor of cardiovascular disease risk than measuring cholesterol, including:
- LDL cholesterol is only one of many components of LDL particles. ApoB reflects the number of LDL particles better than LDL cholesterol.
- Measuring apoB can identify the presence of small, dense LDL particles, which are more atherogenic (i.e., have the ability to build up plaque in blood vessels) than the large LDL particles.
- In some people, LDL cholesterol may be relatively low but may still be high in LDL particles, indicating an increased risk of cardiovascular disease. Measuring apoB can help determine this risk more accurately.
- ApoB is less influenced by nutritional factors, making it better suited as a constant measure for risk assessment.
Measuring apoB is therefore a useful complement to traditional cardiovascular disease risk factors, such as cholesterol and blood pressure, and can help identify individuals at high risk for these conditions. However, it is important to emphasize that no single measurement can determine whether or not a person is at high risk for cardiovascular disease, and that a healthy lifestyle and regular monitoring remain essential to reduce these risks.
InsideTracker incorporates ApoB into their dashboard
InsideTracker is a company that offers personalized health recommendations based on data from blood tests and other biomarkers. The company included ApoB in its test panel because of its important role in determining cardiovascular disease risk.
Measuring ApoB levels can provide information about the total number of LDL cholesterol particles in the blood, which is an important indicator of cardiovascular disease risk. InsideTracker recognizes that measuring ApoB in combination with other markers such as cholesterol, triglycerides and blood pressure can help determine cardiovascular disease risk at the individual level.
In addition, InsideTracker applies advanced algorithms and machine learning to the collected data to provide personalized recommendations to reduce cardiovascular disease risk and improve overall health. By including ApoB in the test panel, InsideTracker can improve the accuracy of their risk assessment and provide clients with better recommendations to improve their health and reduce the risk of cardiovascular disease.
InsideTracker has added ApoB to their "Blood Results Upload" plan , because it provides more context for other lipid markers and allows a more comprehensive analysis of your heart health. Although your biomarkers fall within a certain reference range, this does not always mean you are healthy. Research shows that optimal heart health is associated with ApoB levels below 90 mg/dL.
If your ApoB levels are higher than optimal, InsideTracker gives you science-based recommendations to improve these levels, which in turn can help improve your LDL cholesterol levels.
What exactly are you measuring with ApoB?
Apolipoprotein B (ApoB) is a protein that transports cholesterol on lipoproteins in the blood. There are different types of lipoproteins, such as high-density lipoprotein (HDL), low-density lipoprotein (LDL) and very low-density lipoprotein (VLDL), all of which transport cholesterol. However, ApoB is the main structural component of VLDL, LDL and lipoprotein A. These lipoproteins are potential culprits that can clog arteries and contribute to atherosclerosis.
Atherosclerosis is a condition in which plaques accumulate on the inner walls of arteries. If these plaques accumulate in the heart or brain, it can eventually lead to a heart attack or stroke. ApoB plays an important role in this because it determines the amount of cholesterol that can be deposited in the artery wall. It can be seen as a direct measure of the number of ApoB particles in the bloodstream, which can more accurately predict whether a person is at high risk for heart disease than a calculated measure such as LDL cholesterol, which is based on total cholesterol, HDL cholesterol and triglycerides.
So it is important to know your ApoB level to assess your risk of cardiovascular disease. A high ApoB level can mean insufficient cholesterol is being cleared from the blood, which is often associated with high LDL cholesterol levels. High levels of ApoB and LDL can lead to plaque buildup and narrowing of arteries, which is a risk factor for heart disease.
Can you also get ApoB tested at your doctor's office?
In the Netherlands, general practitioners generally do not offer a standard apolipoprotein B (ApoB) test as part of regular blood tests. GPs will generally evaluate traditional risk factors for cardiovascular disease, such as cholesterol, triglycerides and blood pressure.
However, if a patient is at high risk for cardiovascular disease or if there are other reasons to believe that an ApoB test is necessary, the primary care physician will likely refer the patient to a specialist for the test.
There are several blood tests that can help measure cardiovascular disease risk in addition to cholesterol and apolipoprotein B. Some of these tests include:
1. C-reactive protein (CRP): This is a protein released during inflammation. A high CRP level may indicate an increased risk of cardiovascular disease.
(2) Lipoprotein (a) [Lp(a)]: This is a type of lipoprotein similar in structure to LDL cholesterol. A high level of Lp(a) in the blood is an independent risk factor for cardiovascular disease.
3. Homocysteine: This is an amino acid that in high concentrations in the blood can indicate an increased risk of cardiovascular disease.
Glucose and insulin: Elevated glucose and insulin levels may indicate insulin resistance, which may contribute to an increased risk of cardiovascular disease 4.
5 Triglycerides: These are fat molecules that circulate in the blood. High levels of triglycerides can be a sign of increased risk of cardiovascular disease.
![]()
Cholesterol is an essential molecule produced by every cell in our body and plays an important role in building cell membranes and hormones.
Does eating directly affect your cholesterol levels? It is possible to eat cholesterol-rich foods without the cholesterol we get through our diet remaining in our bodies...,
Although certain foods are rich in cholesterol, the cholesterol present in these foods will not be absorbed directly into our bodies. Instead, the cholesterol we receive through our diet is esterified (bound to fatty acids) in the intestines before being absorbed into the blood. This esterified cholesterol is then excreted by the liver and cannot contribute to the accumulation of cholesterol in the blood vessels. So eating foods that contain cholesterol does not necessarily mean that cholesterol levels in our blood will increase. Some foods do have the potential to stimulate the production of cholesterol in the liver, which can contribute to high cholesterol levels in the blood. LDL and HDL are only lipoproteins that carry cholesterol and are not in themselves a cause of cardiovascular disease. It os important to look at overall health and lifestyle factors such as exercise and diet, rather than focusing only on cholesterol levels.
What should you do in case of an elevated value?
If you want to optimize your ApoB levels, there are several steps you can take. One way to lower your ApoB levels is to eat less saturated fats and more high-fiber foods such as oats and beans. Fiber, especially the soluble fiber found in oats and beans, can remove cholesterol from the body by binding to the cholesterol and pulling it out of the body. In addition, replacing saturated fats, such as those found in cheese, fatty meat, full-fat dairy, and palm and coconut oil, with unsaturated fats, such as olive oil or avocado oil, can help lower your ApoB levels and promote heart health.
To lower the risk of cardiovascular disease, it is generally recommended to follow a diet rich in vegetables, fruits, whole grains, lean proteins (such as poultry, fish, legumes and tofu) and healthy fats (such as nuts, seeds and olive oil). Here are some specific foods you can include in your diet:
- Oily fish, such as salmon and mackerel, which are rich in omega-3 fatty acids
- Whole grain products, such as brown rice, whole grain bread and quinoa
- Fruits and vegetables, especially leafy vegetables and berries
- Nuts, seeds and avocados that are good sources of monounsaturated and polyunsaturated fats
- Legumes, such as chickpeas, lentils and black beans
- Limit intake of processed foods, refined carbohydrates and saturated fats, such as processed meats, fried foods, fast foods and processed snacks.
In addition to diet, regular exercise, a healthy weight, quitting smoking and reducing stress are also important to reduce the risk of cardiovascular disease.
If your ApoB levels are too high, it is important to take steps to lower them. Here are some possible steps you could take:
- Reduce intake of saturated and trans fats: Foods such as red meat, whole dairy products, fried foods and processed foods are high in saturated and trans fats. By reducing your intake of these foods and replacing them with healthier options such as whole grains, vegetables, fruits, legumes, nuts and seeds, you can lower your ApoB levels.
- Increase fiber intake: Fiber is important for reducing cholesterol and ApoB in the bloodstream. You can add fiber-rich foods such as whole grains, fruits, vegetables, legumes, nuts and seeds to your diet.
- Increase intake of healthy fats: Unsaturated fats such as olive oil, avocados, nuts and seeds can help lower ApoB levels. So try to add more of these healthy fats to your diet.
- Increase physical activity: Physical activity can help lower cholesterol and ApoB levels. Try regular exercise, such as walking, jogging, cycling, swimming or strength training.
- Consult your doctor: If your ApoB levels are too high, it is important to consult your doctor. He or she can give you further advice and treatments, such as prescribing medication.
When will you have a good result?
The lab report of Blood Value Test, performed by the certified hospital laboratory Medical Laboratory Dr. Stein & Collegae, indicates that a value between 0.63 and 1.33 g/l is good, but this is the medical result for people who are not sick.
InsideTracker indicates that the optimal value you can achieve by improving your lifestyle should be below 0.71 g/l
The unit of ApoB is usually expressed in milligrams per deciliter (mg/dL) in the United States. However, in Europe and other parts of the world, the unit of grams per liter (g/L) is usually used. To convert ApoB levels from mg/dL to g/L, divide the mg/dL number by 100 because there are 100 mg/dL in 1 g/L.
So for example, if a person's ApoB level is 90 mg/dL, this would correspond to 0.9 g/L (90/100 = 0.9). If you have our Dutch results entered into your Dashboard by InsideTracker, the unit is automatically converted.
![]()
There is no single optimal blood value for ApoB that applies to everyone, as the ideal level depends on several individual factors such as age, gender, medical history, and so on. However, it is generally believed that a lower ApoB level is better for heart health.
ApoB levels below 90 mg/dL (milligrams per deciliter) are generally considered optimal for the prevention of cardiovascular disease, while levels between 90-110 mg/dL are still considered reasonably safe. Higher ApoB levels may indicate a higher risk of cardiovascular disease and should be discussed with a physician to determine a treatment plan.
Note: ApoB is only one of many biomarkers that can be used to assess heart health. A complete evaluation of heart health requires a thorough assessment of all risk factors, including blood pressure, BMI, smoking history, physical activity and cholesterol levels.


